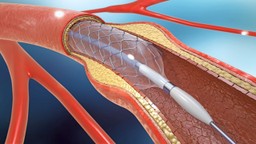
Why Heart Patients Should Get a Stress Test Before an Angioplasty or Stenting
Researchers at University of California at San Fransisco have found that less than half of Medicare patients received noninvasive stress testing prior to elective angioplasty and stenting. Angioplasty and/or stenting are often used to treat angina and ischemia, both of which occur when there is inadequate blood supply to an area of the heart. However, these procedures carry an increased risk of repeat revascularization, late-stent thrombosis (formation of blood clots) and a decreased quality of life if performed in patients with minimal symptoms.
“With the increasingly widespread use of [angioplasty and stenting] in patients with stable coronary artery disease, it is important that these procedures are being done in patients for whom there is reasonable expectation of benefit, patients with documented ischemia or its symptoms,” said Rita Redberg, MD, a cardiologist at UCSF Medical Center and director of Women’s Cardiovascular Services at the UCSF National Center of Excellence in Women’s Health.
“In most patients who are not having a heart attack, a noninvasive stress test should take place before physicians make the decision to go forward with invasive procedures like stenting and angioplasty,” said Grace Lin, MD, associate adjunct professor of medicine at UCSF. “We undertook this study to scrutinize a common procedure to learn how best to direct our resources.”
The researchers found that there was significant geographic variation in the rate of stress testing by hospital referral region, with rates ranging from a low of 22.1 percent to a high of 70.6 percent.
The researchers also found that patients who had a prior cardiac catheterization (the passing of a thin flexible tube into the heart to obtain diagnostic information or to provide treatment) were less likely to undergo stress testing prior to elective angioplasty or stenting.
The team also found that patient characteristics were associated with the likelihood of a patient receiving a stress test prior to angioplasty or stenting. Female sex, age of 85 years or older and having co-existing illnesses such as rheumatic disease, chronic obstructive pulmonary disease, congestive heart failure and coronary artery disease were associated with a decreased likelihood of stress testing prior to angioplasty or stenting. Yet, being of the black race and having a history of chest pain was associated with an increased likelihood of a stress test prior to angioplasty or stenting.
Patients of physicians who performed a higher volume of angioplasty and stenting procedures had slightly lower rates of stress testing. No hospital characteristics were associated with whether patients received stress testing, but taken together, hospital factors such as type of equipment, whether the facility had a catheterization laboratory, a cardiac surgery program or whether it was a teaching hospital did associate with a higher likelihood of stress testing.
“This tells us that where you live, who you see, what race and gender you belong to and what type of facility exists in your area affects whether you will have a stress test prior to receiving a stent or angioplasty.” Lin said. “We want to understand why physicians make the decisions they make so we can improve care and encourage more evidence-based practice. Further studies will help elucidate these questions.”
If you or someone you love suffered an injury during an angioplasty or stenting procedure there may be medical malpractice behind the injury. Contact the lawyers at Berger & Lagnese, LLC for a free consultation. Let the lawyers at Berger & Lagnese, LLC help you find out whether medical malpractice is to blame for your angioplasty- or stent-related injury.